Ectopic Pregnancy – Understanding the “Different Type” of Pregnancy

An ectopic pregnancy is a serious condition in which a fertilized egg implants outside the uterus, rather than inside it.
The term “ectopic” comes from the Greek word “ectopos”, meaning “in the wrong place.”
In a normal pregnancy, the sperm fertilizes the egg in the fallopian tube, and the embryo travels to the uterus for implantation and growth.
However, in an ectopic pregnancy, the fertilized egg gets stuck—most often in the fallopian tube—and starts developing there or in other locations such as the ovary, cervix, or abdominal cavity.
Although relatively rare, it occurs in 1–2 out of every 100 pregnancies.
If not diagnosed and treated early, it can cause severe internal bleeding and become life-threatening for the mother.
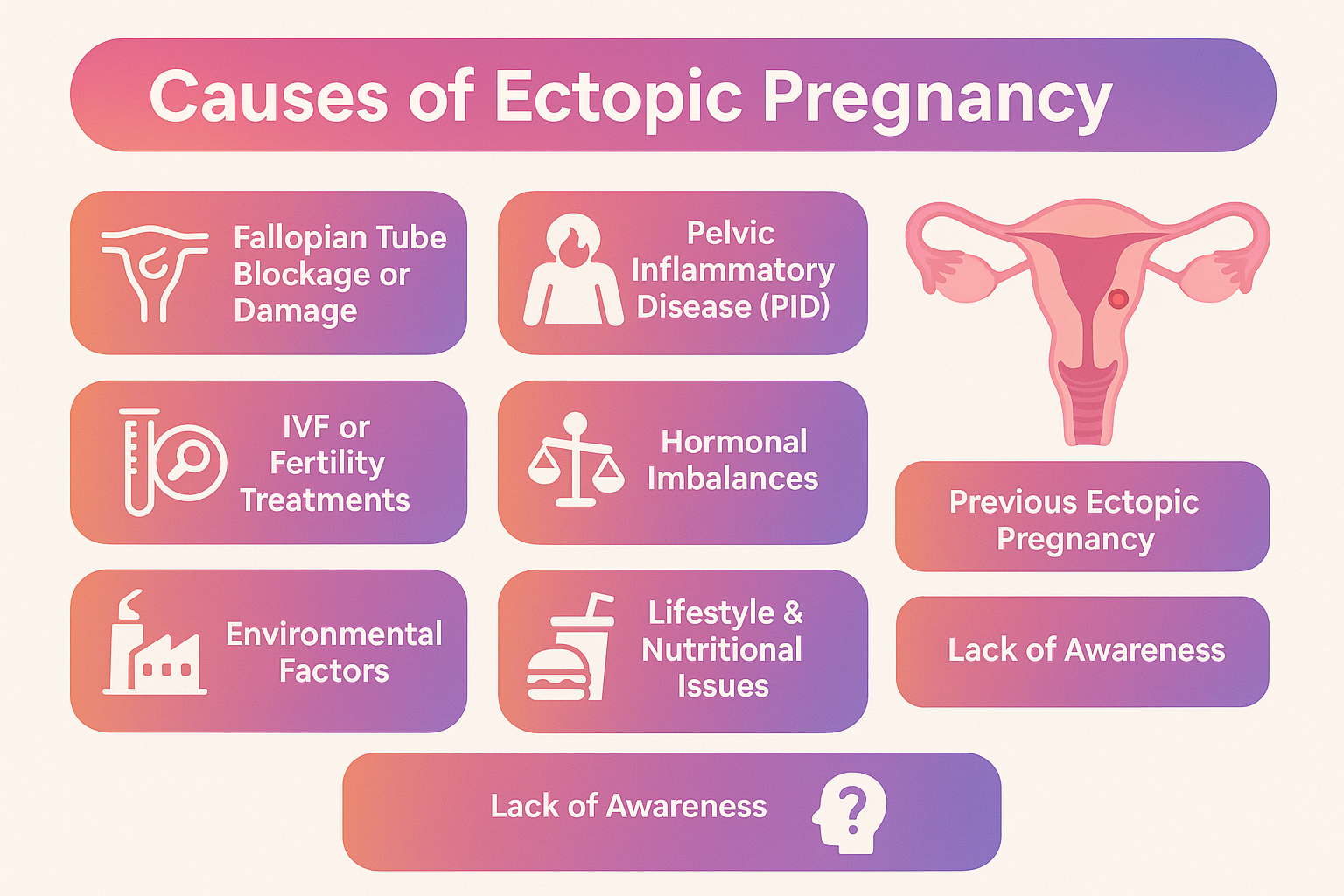
Causes of Ectopic Pregnancy
Get routine gynecological and pelvic health screenings to detect infections or blockages early.
There are several medical, lifestyle, and environmental factors that can increase the risk of ectopic pregnancy:
-
Fallopian Tube Blockage or Damage – Due to infection, inflammation, or prior surgery.
-
Pelvic Inflammatory Disease (PID) – Damages the tube’s inner lining, preventing the embryo from reaching the uterus.
-
Previous Ectopic Pregnancy – A history of one increases the risk of recurrence.
-
IVF or Fertility Treatments – Occasionally, during assisted reproduction, the embryo may implant outside the uterus.
-
Hormonal Imbalances – Irregular hormone levels can interfere with egg movement.
-
Substance Abuse – Smoking, alcohol, or drug use can affect fertility and tubal health.
-
Environmental Factors – Exposure to radiation, harmful chemicals, or X-rays.
-
Lifestyle & Nutritional Issues – Deficiency of folic acid or vitamin B, obesity, and poor diet.
-
Lack of Awareness – Many women, especially in rural areas, are unaware of the symptoms and risks of abnormal pregnancies, leading to delayed diagnosis.
How to Identify an Ectopic Pregnancy (Diagnosis)
Prevent sexually transmitted infections (STIs) by maintaining hygiene and using protection.
Early diagnosis is crucial for safety and treatment. Doctors use multiple methods to confirm the condition:
1. Medical History & Symptoms
The doctor begins by asking key questions such as:
-
When was your last menstrual period?
-
Is your pregnancy test positive?
-
Do you experience sharp pain on one side of the lower abdomen?
-
Any history of pelvic infections, surgeries, or abortion?
These details help differentiate a normal pregnancy from an ectopic one.
2. Pregnancy Tests
a. Urine Pregnancy Test –
Detects hCG (human chorionic gonadotropin) hormone.
If the test is positive but no pregnancy sac is visible in the uterus, it may indicate an ectopic pregnancy.
b. Blood hCG Level –
In a normal pregnancy, hCG levels double every 48 hours.
In an ectopic pregnancy, levels rise slowly or remain constant.
If hCG >1500 IU/L but no embryo is seen in the uterus via ultrasound, it confirms ectopic pregnancy.
3. Transvaginal Ultrasound (TVS)
This is the most important test for diagnosis.
A small ultrasound probe is inserted into the vagina to obtain clear images of the uterus, ovaries, and fallopian tubes.
It helps check:
-
Whether the gestational sac is in the uterus
-
Presence of abnormal mass or fluid in the fallopian tube
-
Signs of internal bleeding
If the uterus is empty and a mass with fluid (blood) is seen near the tube, an ectopic pregnancy is confirmed.
4. Progesterone Level Test
In a healthy pregnancy, progesterone levels are typically 25 ng/ml or higher.
If levels fall below 5 ng/ml, it may suggest an abnormal or ectopic pregnancy.
5. Laparoscopy
When ultrasound and blood tests don’t provide clear results, doctors perform a diagnostic laparoscopy.
A small camera (laparoscope) is inserted through a tiny incision in the abdomen to view the uterus, fallopian tubes, and ovaries directly.
This method allows doctors to diagnose and treat the ectopic pregnancy simultaneously.
Why Is Ectopic Pregnancy Becoming More Common?
Include foods rich in iron, folic acid, and vitamin B to support reproductive health
Modern lifestyle and health factors are contributing to the increasing number of ectopic pregnancies, including:
-
Higher rates of Pelvic Inflammatory Disease and sexually transmitted infections
-
Delayed pregnancies due to career and lifestyle priorities
-
Frequent use of assisted reproductive techniques (IVF, IUI)
-
Increased smoking and alcohol use
-
Poor nutrition and sedentary habits
These factors can affect fertility, hormonal balance, and reproductive health, making women more susceptible to complications.

⚠️ Warning Signs of an Ectopic Pregnancy
Understand your body and menstrual cycle. Seek medical help immediately if you notice pain, spotting, or irregular symptoms during early pregnancy.
Recognizing early symptoms can be lifesaving. Seek medical attention immediately if you experience:
-
Severe pain on one side of the lower abdomen
-
Spotting or vaginal bleeding (especially during early pregnancy)
-
Pain in the shoulder or neck, which may indicate internal bleeding
-
Dizziness, nausea, or weakness
-
Fainting or signs of hemorrhagic shock in severe cases
💡 If you notice any of these symptoms, seek emergency medical care immediately.
🌿 How to Reduce the Risk of Ectopic Pregnancy
-
Prevent Sexually Transmitted Infections (STIs)
Unsafe sex can lead to infections like chlamydia and gonorrhea, which cause Pelvic Inflammatory Disease (PID)—a major risk factor for ectopic pregnancy.
👉 Always practice safe sex and maintain good personal hygiene. -
Avoid Smoking
Smoking reduces blood flow and affects the health of fallopian tubes, increasing the risk of complications. -
Adopt a Healthy Lifestyle
Eat nutritious foods rich in folic acid, iron, and vitamins. Avoid junk food and maintain a healthy weight. -
Exercise Regularly
Gentle yoga, stretching, and regular exercise improve blood circulation and reproductive health. -
Get Regular Checkups
Routine pelvic examinations and ultrasounds help detect early infections or abnormalities. -
Manage Stress
Chronic stress can affect hormonal balance and reproductive health. Practice meditation or breathing exercises to stay calm. -
Inform Your Doctor of Past Ectopic Pregnancy
If you have had an ectopic pregnancy before, inform your healthcare provider before planning another pregnancy. This helps in early monitoring and risk prevention.

Final Thoughts
An ectopic pregnancy is a medical emergency—but with early diagnosis, awareness, and timely intervention, it can be managed safely.
If you experience severe abdominal pain, bleeding, or faintness during early pregnancy, seek medical attention immediately.
Awareness, preventive care, and regular health checkups can help protect women from the life-threatening risks of ectopic pregnancy and support safer motherhood.